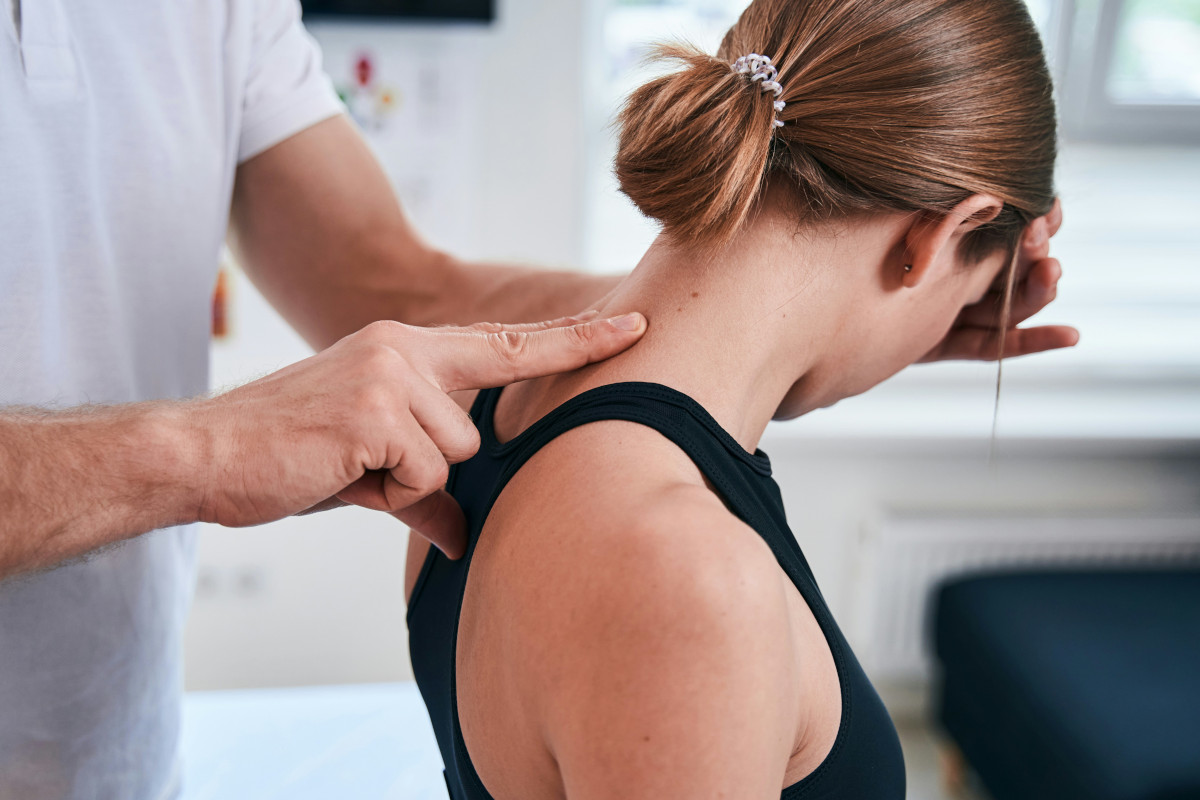
Migraine and our sense of smell — more about an astonishing connection
What we smell affects how we experience pain. This connection has been known for thousands of years – even the ancient Egyptians wrote about it. However, research into the precise causes of the phenomenon is fairly new. Groundbreaking discoveries in this field were made by American scientists Richard Axel and Linda Buck, who were awarded the Nobel Prize in Medicine in 2004 for their work on our sense of smell. They found out that special cells in the lining of the nose are responsible for the human sense of smell. These sensory cells are directly linked to the so-called olfactory bulb. Interestingly, this 'smell centre' is also connected to brain regions responsible for memory, emotions, and our sensitivity to pain.
-
References
Aktürk T, Tanık N, Serin Hİ, Saçmacı H, İnan LE. Olfactory bulb atrophy in migraine patients. Neurol Sci. 2019 Jan;40(1):127-132. doi: 10.1007/s10072-018-3597-6. Epub 2018 Oct 2. PMID: 30280362.
Buck L, Axel R. A novel multigene family may encode odorant receptors: a molecular basis for odor recognition. Cell. 1991 Apr 5;65(1):175-87. doi: 10.1016/0092-8674(91)90418-x. PMID: 1840504.
Doğan A, Bayar Muluk N, Şahan MH, Asal N, Inal M, Ergün U. Olfactory bulbus volume and olfactory sulcus depth in migraine patients: an MRI evaluation. Eur Arch Otorhinolaryngol. 2018 Aug;275(8):2005-2011. doi: 10.1007/s00405-018-5029-x. Epub 2018 Jun 6. PMID: 29876641.
Gossrau G, Frost M, Klimova A, Koch T, Sabatowski R, Mignot C, Haehner A. Interictal osmophobia is associated with longer migraine disease duration. J Headache Pain. 2022 Jul 15;23(1):81. doi: 10.1186/s10194-022-01451-7. PMID: 35840888; PMCID: PMC9284850.
Lötsch J, Hähner A, Gossrau G, Hummel C, Walter C, Ultsch A, Hummel T. Smell of pain: intersection of nociception and olfaction. Pain. 2016 Oct;157(10):2152-2157. doi: 10.1097/j.pain.0000000000000599. PMID: 27152690.
Mignot C, Faria V, Hummel T, Frost M, Michel CM, Gossrau G, Haehner A. Migraine with aura: less control over pain and fragrances? J Headache Pain. 2023 May 17;24(1):55. doi: 10.1186/s10194-023-01592-3. PMID: 37198532; PMCID: PMC10189721.
Rottstaedt F, Weidner K, Strauß T, Schellong J, Kitzler H, Wolff-Stephan S, Hummel T, Croy I. Size matters - The olfactory bulb as a marker for depression. J Affect Disord. 2018 Mar 15;229:193-198. doi: 10.1016/j.jad.2017.12.047. Epub 2017 Dec 28. PMID: 29324366.
Schlenger, R.L. Geruchssinn und Migräne: Wenn der Schmerz zu riechen ist. Dtsch Ärztebl 2021; 118(50): A-2398 / B-1965.
Silva-Néto RP, Rodrigues ÂB, Cavalcante DC, Ferreira PH, Nasi EP, Sousa KM, Peres MF, Valença MM. May headache triggered by odors be regarded as a differentiating factor between migraine and other primary headaches? Cephalalgia. 2017 Jan;37(1):20-28. doi: 10.1177/0333102416636098. Epub 2016 Sep 30. PMID: 26924838.
Sjöstrand C, Savic I, Laudon-Meyer E, Hillert L, Lodin K, Waldenlind E. Migraine and olfactory stimuli. Curr Pain Headache Rep. 2010 Jun;14(3):244-51. doi: 10.1007/s11916-010-0109-7. PMID: 20490744.
Weiss J, Pyrski M, Jacobi E, Bufe B, Willnecker V, Schick B, Zizzari P, Gossage SJ, Greer CA, Leinders-Zufall T, Woods CG, Wood JN, Zufall F. Loss-of-function mutations in sodium channel Nav1.7 cause anosmia. Nature. 2011 Apr 14;472(7342):186-90. doi: 10.1038/nature09975. Epub 2011 Mar 23. PMID: 21441906; PMCID: PMC3674497.
Zufall F, Pyrski M, Weiss J, Leinders-Zufall T. Link between pain and olfaction in an inherited sodium channelopathy. Arch Neurol. 2012 Sep;69(9):1119-23. doi: 10.1001/archneurol.2012.21. PMID: 22733046.